When you are sick, you want medical care right away. In traditional clinics, that might not be possible, but clinics like the South Arkansas Medical Associates (SAMA) Healthcare Services in El Dorado are delivering healthcare differently, and more efficiently, through a public-private partnership championed by Arkansas Blue Cross and Blue Shield – the Comprehensive Primary Care (CPC) initiative.
CPC+ is a program of the Centers for Medicare and Medicaid Services (CMS) that rewards primary care clinics for achieving better outcomes and invests in new ideas to improve health. The program, now in its second phase, was introduced in Arkansas in 2012.
CPC initiative helps SAMA deliver better patient access, health outcomes
How big of a difference did CPC make? Here are a few highlights:
- The rate of uncontrolled diabetes has been cut in half
- Uncontrolled high blood pressure is falling almost as dramatically
- Hospital admission and emergency room visit rates are several times lower than the national average
- Access for same-day appointments has doubled
- Quality measures have improved each year
- Employee satisfaction is up, and turnover is down
- South Arkansas Medical Associates clinic in El Dorado, Arkansas.
- This patchwork quilt wall-hanging was inspired by SAMA’s color-coded care teams.
- SAMA CEO Pete Atkinson says CPC was a turning point.
- Staff work around the purple team’s station.
- Clinic staff confer in the in-house pharmacy.
Before CPC
“We were functioning as four individual medical practices operating under one roof,” said Pete Atkinson, the clinic’s chief executive officer. “Patients had only a 25% chance of seeing their designated primary care physician. We were booked solid and stretched thin. Our entire staff was in ‘survival mode.’ But we only had so much money to spend, so our staffing capacity was limited.
Matthew Callaway, M.D., a founding SAMA physician, was battle-weary as well. “We had the computer power but not the manpower,” he said. “The focus was on trying to take care of today’s problem. We had trouble tracking patients and keeping tabs on the results of visits to specialists or doing standard health maintenance – like follow-ups on A1c (blood sugar) levels and so forth.”
The transformation
CPC’s shift to a value-based system allowed SAMA to try things the way the staff had always wanted to.
Atkinson used CPC-provided value payments to hire four nurse practitioners, four nurse care managers and four staff nurses. He then, “literally overnight,” reorganized the staff into four teams, with a physician, a nurse practitioner and three nurses on each team. Each color-coded team was assigned to one-quarter of the clinic’s 22,000 patients. The décor of each team’s area matches its assigned color, down to the color of each team’s uniforms. Later, a population health nurse was added to identify trends among the clinic’s overall patient base and advise care managers on the management of at-risk patients.
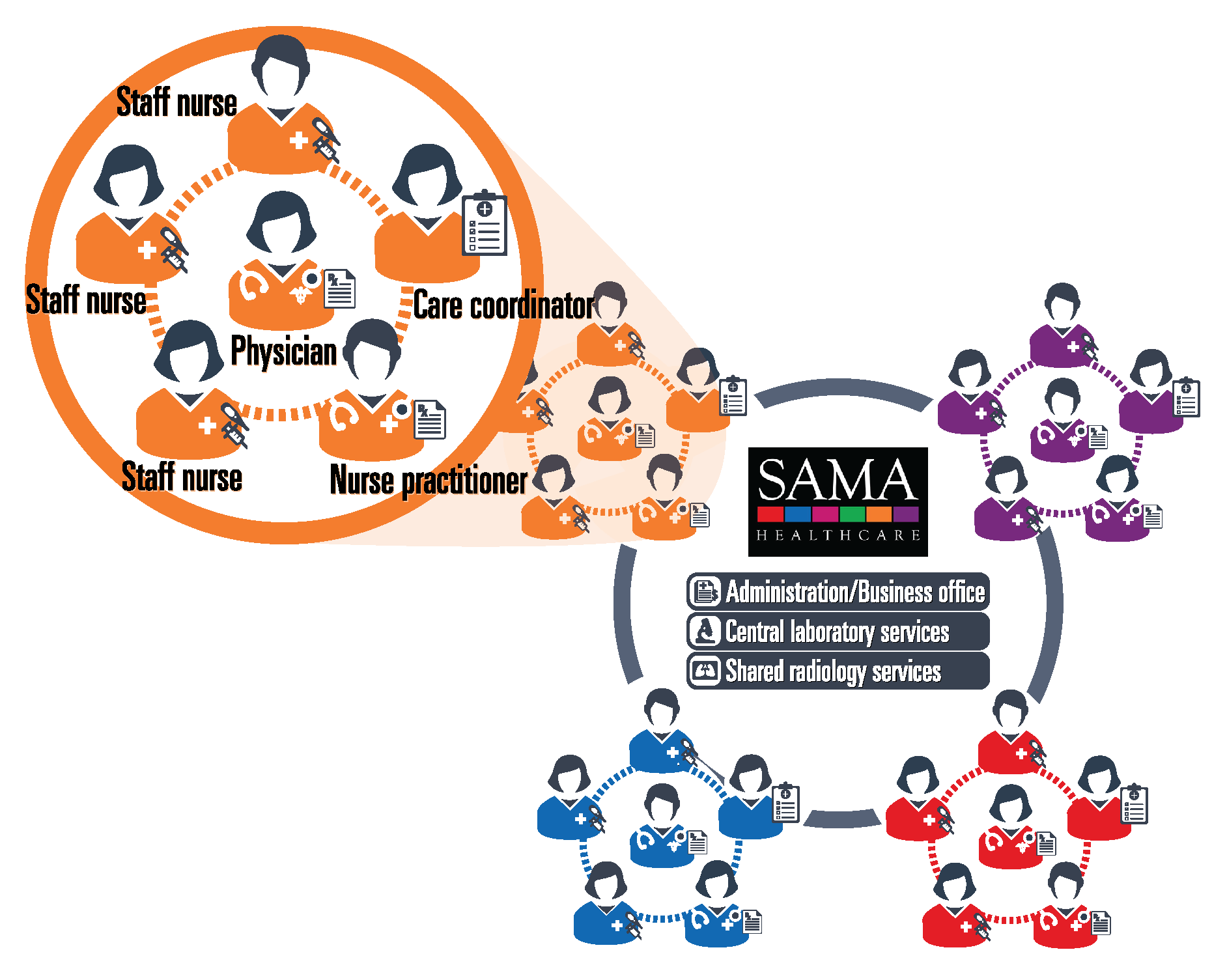
The results
Atkinson says this arrangement ensures that patients are seen by their assigned care team “about 90% of the time.” Doctors see fewer patients and spend more time with each patient. Teams have a greater ability to check in with patients, educate them and monitor their conditions.
For example, patients who have been hospitalized or seen in an ER get a call within 24 hours and have a follow-up visit within a week.
“Not a person here – from the physicians to the front desk – would go back to the way things were before,” Atkinson said.
Dr. Callaway agrees: “It really loosened us up to do things we always wished we could do but didn’t have the resources to get done.”
Atkinson said the change was so noticeable that a year after the reorganization, “a nurse practitioner and physician walked in our door and said they wanted to join us. They became the green team.”
Susan Taylor, R.N., SAMA’s population health manager, says patients and staff have responded to the change: “Patients love the change. Wellness visits continue to grow. Patients actually call us when it’s been a year. We are extremely proud, on a personal level, of what we can get done as a team,” she added. “What we have been able to do through CPC is the way healthcare always should have been.”