Medicare supplement members receive more “reader-friendly” documents
Medi-Pak® Medicare supplement members got an upgrade!
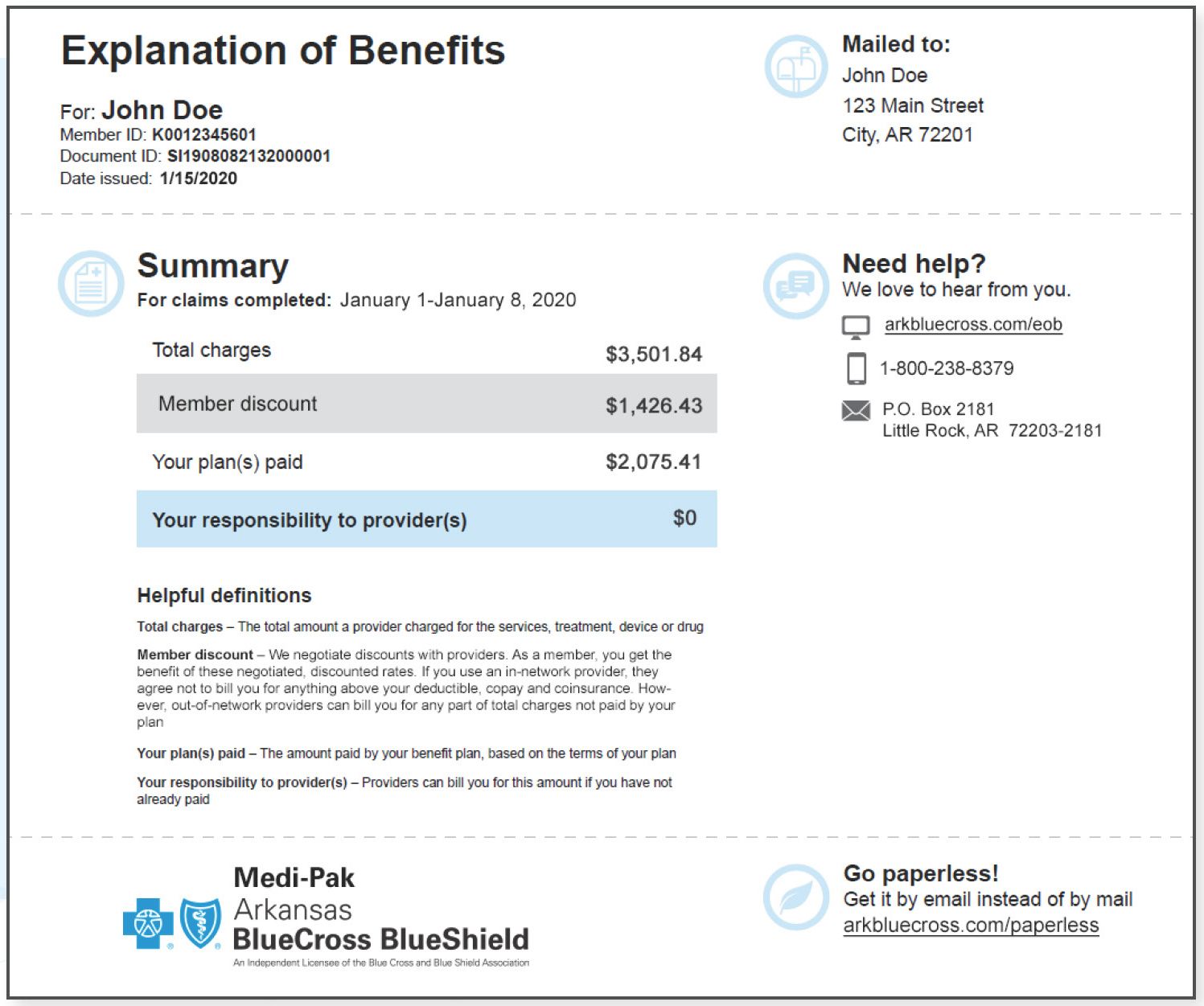
As a Medi-Pak member, you’re now receiving an easier to read and understand Explanation of Benefits (EOB). Your EOB details how your healthcare claims were paid. And, it helps you track your healthcare claims history as well as any amounts that remain to be paid to healthcare providers. Remember: an EOB is not a bill.
Additionally, you’ll see each page groups your medical charges by a healthcare provider. Best of all, throughout your EOB, you’ll find definitions to help explain any confusing terminology.
In the past, members received claims documents one time each month. Now Medi-Pak members receive their EOB every two weeks if you’ve had a healthcare claim processed during that time.
The cover page summarizes:
- The amount your provider(s) charged
- How much Arkansas Blue Cross, Medicare and/or other coverage paid
- What (if anything) you owe to your healthcare provider(s)
If you have any questions about the new EOB format, give us a call at 1-800-338-2312, 8 a.m.-5 p.m. Monday-Friday.

